CDHB
Studies have shown that up to 50% of patients on admission to hospital have evidence of protein energy malnutrition caused by reduced nutrient intake. Nutrition support is the provision of nutrients orally, enterally, or parenterally with therapeutic intent.
Nutrition support is individualized, based on a formal nutritional assessment and concomitant factors such as disease state, organ function, metabolic condition, electrolyte measurements, medication use, and duration of nutritional support proposed.
Standard parenteral nutrition (PN) consists of 1.5, 2, and 2.6 L bags containing glucose (200-320 g), amino acids (60-100 g), lipid emulsion (60-100 g), electrolytes, trace elements and multivitamins. Non-standard bags are also available at a higher cost.
PN may be required where enteral nutrition is not possible. This is likely to occur in the following circumstances:
PN is an expensive therapy with risks to the patient. PN of less than 5 days is unlikely to benefit the patient.
PN can be initiated once a peripherally inserted central catheter (PICC) or other central venous catheter has been placed and the Nutrition Support Team (pager 8944) or the ward dietitian has been consulted. PN is initiated at half rate for the first 6 hours. If blood glucose levels are satisfactory, and the patient is not at risk of refeeding syndrome, increase to full rate as determined by the dietitian.
Bloods for biochemistry should be taken at approximately 18:00 hours when the PN bag is changed. This expedites the writing of the following day's prescription, which must be faxed to the pharmacy by 10:00 am.
Further useful information on nutrition support is available on general surgical wards and in ICU, CHOC, BMTU, Ward 26, and on the CDHB intranet (search for "TPN prescribing").
If in doubt, contact the Nutrition Support Team (pager 8944) or your ward dietitian.
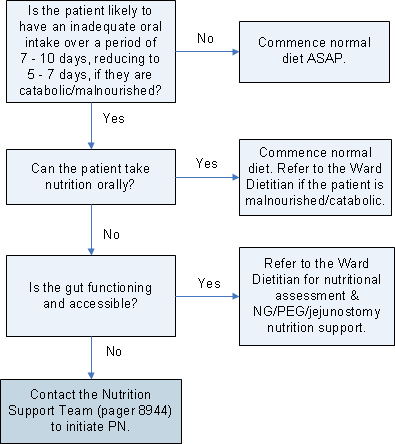
Medical Review of Patient's Nutritional State
Medical Review of Patient's Nutritional State

Notes:
Topic Code: 3580