CDHB
Respiratory failure is defined as occurring with PaO2 <60 mm Hg, or PaCO2 >50 mm Hg in a patient at rest breathing air. Respiratory failure is not a disease but reflects the inability of the lungs to maintain normal gas exchange.
Note: A kilopascal (kPa) is the SI unit of pressure. 1 mm Hg equals 0.13 kPa and 1 kPa equals 7.5 mm Hg.
Both types of respiratory failure may be acute or chronic.
Patient assessment: The underlying cause for the respiratory failure must be determined to enable appropriate treatment in each case.
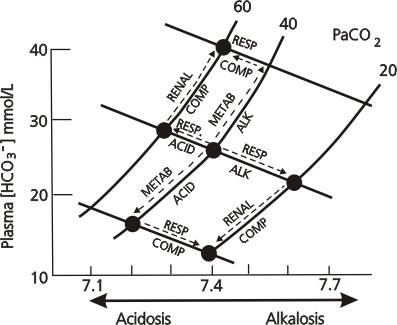
Blood gas interpretation may be assisted by the following diagram (which is also discussed under Acidosis / Alkalosis):

Calculation of the A-a gradient assists in differentiating between hypoventilation and V/Q mismatching as the source of hypoxaemia. It predicts the degree of shunt by comparing the partial pressure of O2 in the (A) alveoli to that in the (a) artery. The difference between them gives us an idea how well the oxygen is moving from the alveoli to the arterial blood.
Normal A-a gradient for a young adult is <20. The A-a gradient increases with age. For elderly patients (>75 yrs) a normal A-a gradient is <25.
Calculation of the A-a Gradient
Calculation of the A-a Gradient |
A-a Gradient = PAO2 - PaO2 |
|
Estimation of PAO2 |
PAO2 = PiO2 - PaCO2/R |
|
Note: A-a gradient is best calculated from a blood gas taken on room air (FiO2 = 0.21). Whilst on supplemental oxygen it is usually difficult to obtain an accurate assessment of FiO2 due to variability in actual % of oxygen delivery.
Topic Code: 1624